“When you’re told that nothing can be done, no treatment, no cure. It’s a case of being made comfortable to see it out. The idea of chemotherapy is amazing; you get the opportunity to fight back.”
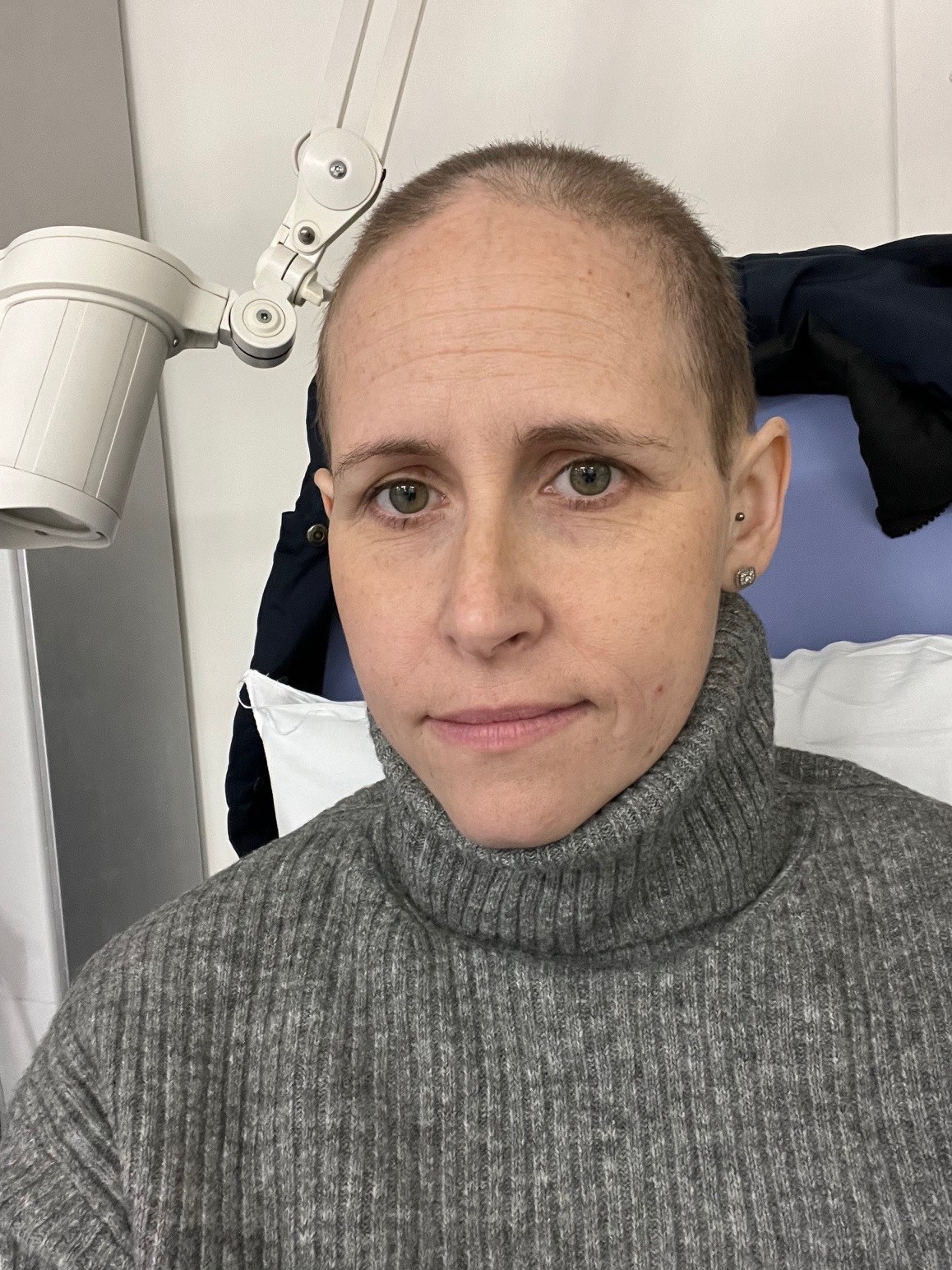
Charlie Anderson-Read was diagnosed with pancreatic cancer in November 2023, she has been fighting ever since and she is here today to tell you her story.

It all started in early July 2023, when I was dealing with something stressful at work. A colleague brought me breakfast, and I couldn’t stomach it. I put it down to the stressful situation I was in. Then, over the next few weeks, my appetite slowed, and I couldn’t eat as much as I used to. Again, I put it down to stress. During that time, my dad was diagnosed with terminal cancer.
Over the next few weeks, I slowly developed a slight pain in my left side. I could feel a very slight hard area when I laid down where it very occasionally hurt. The pain wasn’t constant, but it would heighten when I was thinking about my dad or when I was seeing him in the hospital. Sometimes, I couldn’t stand up straight, but this wasn’t always the case, and it would settle when I was out of a stressful situation.
Then in August 2023, I contacted occupational health through work. I wanted to get my stress under control so it wouldn’t affect my work. In my mind, I didn’t feel stressed, but I thought it had manifested physically instead. They told me it was probably stress but to go to my GP, just in case.
I did, and I got a very quick appointment the same morning. When the GP examined me, he couldn’t identify the hard area in my abdomen that I described. He said it was likely stress and asked what I wanted from the appointment. He referred me for blood work just in case it was anything else. The results showed high levels of alkaline in my liver but not much else.

I was sent for an ultrasound scan at the beginning of November 2023. The following week the GP rang me and said it was very serious. He said he suspected I had some form of cancer, and I was booked in for an urgent CT scan.
Over the next few days, my symptoms got increasingly worse, and two weeks was too long to wait because I was deteriorating so quickly. Due to the pain I was suffering, and the fact I was struggling to stand up straight or walk, I self-presented at A&E in Bristol.
I was seen quickly; I think they recognised how bad it was. They did blood tests, and I had an ECG. They confirmed that I didn’t have organ failure, and they debated whether they would send me for a CT scan. However, because they were in a different NHS trust to where I was being treated, they said they would have to start the investigation from the beginning as they didn’t have access to my records. They released me with pain relief.
The next day, I felt worse still, so I rang 111 and pushed for an appointment with Urgent Care (They tried to refer me to my GP). I attended Urgent Care in the right NHS trust area. Initially, the nurse couldn’t understand why I had attended hospital. When she looked further into my notes, she could see that professionals were discussing bringing my CT scan forward (something I was unaware of), and I received a CT scan that evening.
In the early hours of the next morning, a surgeon sat me down. I was told I had pancreatic cancer, and it had spread to my liver. It was terminal, and there was nothing that could be done. It was unlikely I would get a biopsy because there were no treatment options.
I said to the doctor: “You must be 100% sure to tell me that there is nothing that can be done.” She pulled a grimace and quietly nodded in agreement. When my dad was diagnosed with terminal cancer, towards the end he knew how long he had to live. I was with him when the doctor told him how long he had, and I saw the look on his face. I decided right then, that if I were ever in the same circumstance, I wouldn’t want to know. It wouldn’t be helpful to me or my family.
Luckily, someone else looked at my CT scan, and I was given a biopsy the following week. I was told there was a very small chance I may be able to have treatment, but if so, it would only extend my life; there was no cure. That Friday morning, my case was discussed by some medical professionals, and I was contacted by a professor, who said there might be a treatment option for me.
“When you’re told that nothing can be done, no treatment, no cure. It’s a case of being made comfortable to see it out. The idea of chemotherapy is amazing; you get the opportunity to fight back.”
I met with him the same day, and after a quick conversation, he authorised two rounds of chemotherapy. He said there was a very small chance it might not be pancreatic cancer, and if so, chemotherapy would be effective in this different form. If it was going to work, he told me, we’d know soon after treatment, but I needed to start it as soon as possible. He booked me in to have my PICC line put in on Monday to start my first course of chemotherapy on Tuesday.
After the first two rounds of chemotherapy, I was examined, and my doctor was surprised to find that it had reduced the size of the tumour. He told me it wasn’t the other form of cancer he suspected it may have been, but, due to the effectiveness of the treatment, he ordered another two rounds.

Without a shadow of a doubt, the chemotherapy has given me so much more quality of life. Yes, I do get mouth and throat ulcers from it, and the days after treatment are a struggle. But, thanks to all the support from my friends and family, it has been so much easier to cope with, and I now have a week leading up to my next course of chemotherapy where I can even go for a little run, which is amazing. My pain has even reduced to the point where I barely need to take painkillers to control the symptoms.
I speak to my professor every three weeks, alternating in person and over the phone. I was initially under the palliative team, but I have since been reassigned directly to my professor. The palliative team said: “Get back in contact with us if you need us”, which was the best news I have got.
In a way, I have been lucky, but if I had waited for my CT scan and hadn’t pushed back, then I think I wouldn’t have been strong enough for the chemotherapy, and I wouldn’t be here today. The professor has since authorised another four rounds of chemotherapy, giving me eight in total. I know that this isn’t a cure, and after my sixth round, I will have another CT scan to see what the treatment has done, and I will then discuss what the next steps will be.
For now, I am living as much life as I can and spending as much time with my daughter and wife as possible. I’m lucky chemotherapy has extended my life, something which I initially didn’t think was possible and for that, I’m so grateful to everyone.
