Second Line Investigations
Second line investigations are often more invasive tests for pancreatic cancer or tests that take longer to complete. They are often more specific than first line investigations and may tell doctors more about the size and stage of a tumour if one has been identified in a first line investigation.
Endoscopy
An endoscope is a long, thin tube with a light and a camera at the end. It is passed down your throat and into your digestive system. An endoscopy can show blockages or swelling in the pancreatic ducts and allows the doctor to judge whether these problems are caused by cancer or not. During the procedure, doctors can also take samples of the tissue or fluid to help them find out if you have cancer. This is also called a biopsy.
The day before your endoscopy, you may need to attend a pre-admission clinic so that some blood can be taken for tests. You will need to tell staff if you suffer from diabetes, glaucoma or take Warfarin.
You must have nothing to eat or drink for at least six hours before your test.
A dye may be injected into the pancreatic bile ducts via an endoscope so that these organs can be viewed as x-ray pictures, known as cholangiograms. This procedure is known as endoscopic retrograde cholangiopancreatography (ERCP). You will also likely be under sedation throughout the procedure.

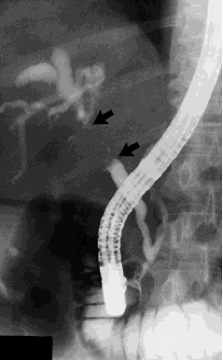
An ERCP X-ray
The doctor will pass the endoscope tube down your oesophagus (the tube that carries food and drink from your throat to your stomach). The tube then passes into the first part of your small bowel (the duodenum), where the opening to the ducts leading to the liver and pancreas are. The doctor then passes a narrow plastic tube, called a catheter, down through the endoscope and into this opening.
The doctor will then inject an X-ray dye through the catheter so that the bile ducts and the pancreas can be seen clearly on the X-ray. The dye used is harmless and will pass out of your body naturally. If the doctor sees a narrowing, he/she can put a small plastic tube, called a stent, into the bile duct to drain the bile into the duodenum and relieve called a stent, into the bile duct to drain the bile into the duodenum and relieve the blockage. If the bile has not been able to drain properly, you may be jaundiced.
 If the doctor sees any abnormalities, a biopsy will be taken. Cell samples, called “brushings”, can also be taken from inside the small ducts. The biopsies and/or cell samples will be sent to the pathology department and examined closely under a microscope. It will take several days before If the doctor sees any abnormalities, a biopsy will be taken. Cell samples, called “brushings”, can also be taken from inside the small ducts. The biopsies and/or cell samples will be sent to the pathology department and examined closely under a microscope. It will take several days before the results are known. The doctor may take some photographs of the area for closer examination later. The test can take between 30-90 minutes.
If the doctor sees any abnormalities, a biopsy will be taken. Cell samples, called “brushings”, can also be taken from inside the small ducts. The biopsies and/or cell samples will be sent to the pathology department and examined closely under a microscope. It will take several days before If the doctor sees any abnormalities, a biopsy will be taken. Cell samples, called “brushings”, can also be taken from inside the small ducts. The biopsies and/or cell samples will be sent to the pathology department and examined closely under a microscope. It will take several days before the results are known. The doctor may take some photographs of the area for closer examination later. The test can take between 30-90 minutes.
You can expect to stay in the hospital overnight, especially if you have had a stent put in. If you are allowed home on the same day as the test, then you will need someone to look after you for the next 24hours. It takes this long for the sedation to leave your system and during this time you must not drive or operate heavy machinery, make any important decisions, or take any alcohol.
Endoscopic Ultrasound
(EUS)Endoscopic ultrasound (EUS) is a type of endoscopy where the doctor uses a thin flexible camera with a small ultrasound probe at the tip. During the test, the doctor will look at the lining of your pancreas, as well as examine the lymph nodes (A small bean-shaped structure that is part of the body’s immune system). Everything will be magnified on a television screen and images will also appear on the ultrasound machine.
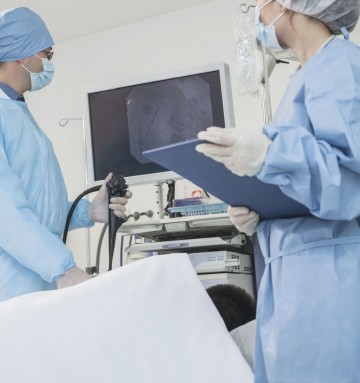 If necessary, your doctor will take samples of cells from the surrounding areas, by means of a fine needle aspiration (FNA) and send them to the laboratory for examination.
If necessary, your doctor will take samples of cells from the surrounding areas, by means of a fine needle aspiration (FNA) and send them to the laboratory for examination.
You cannot eat or drink for several hours before an endoscopy. You will have a sedative and local anaesthetic to make you feel as comfortable as possible. The test should take between 20 and 45 minutes.
If you have had biopsies taken it may take 7 to 10 days before the results are available. Before you leave the hospital after your endoscopy make sure you have an appointment to come back and see your doctor for the results
If, after the procedure, you develop a high temperature, have difficulty swallowing or have increasing throat or chest pain, contact your doctor immediately.
MRI Scan for pancreatic cancer
An MRI (Magnetic Resonance Imaging) produces detailed pictures of the body. Instead of x-rays, it uses a large magnet and radio waves that are fed into a computer. The computer then builds up cross-sectional images of your body. If you need an MRI scan, more written information will be available from your local scanning department.
There is no special preparation for an MRI. However, because of the powerful magnet used to produce the scans, safety guidelines must be followed. You may have to fill in a questionnaire before the scan can be carried out.
It may not be possible to have an MRI scan if you have:
- A heart pacemaker,
- Some types of surgical clips inside your head,
- Metal fragments in your eyes or elsewhere,
- Neuron-stimulator implants.
Please tell your doctor or nurse if you:
- Have any allergies,
- Have asthma,
- Have diabetes,
- Have kidney problems,
- Are taking any medication,
- Are pregnant,
- Have had any surgery in the past 12 weeks,
- Are you in any doubt about your suitability for an MRI scan,
- Have had any problems previously with any type of x-ray or radiology examination.
What will happen?
For the scan:
- Wear something loose without metal zips or buttons.
- Remove all metal objects, including rings, before scanning.
- Remember to check that you do not have any credit cards in your pockets as the magnetic strip is affected by the scan.
 If necessary, you will have an injection of dye into a vein in your arm. This can help improve the images. You will be asked to lie on a table which then moves into the scanner, shaped like a tunnel. The table contains the magnet and the part of your body to be scanned lies directly over its centre. During the scan, you won’t be able to feel anything, but there will be quite a lot of noise. You may be given headphones or earplugs to help with this.
If necessary, you will have an injection of dye into a vein in your arm. This can help improve the images. You will be asked to lie on a table which then moves into the scanner, shaped like a tunnel. The table contains the magnet and the part of your body to be scanned lies directly over its centre. During the scan, you won’t be able to feel anything, but there will be quite a lot of noise. You may be given headphones or earplugs to help with this.
An MRI scan usually takes about 20-30 minutes. It is important to keep still throughout the scan. The radiographer will be outside the room, but you can talk with them through a microphone. You may be able to bring a friend or relative with you when you go to the clinic. They can wait in the waiting room while you have your scan. Please check with the radiology department first in case the clinic is very busy.
At the end of the scan, there will be multiple images for the radiologist to look at. Once these have been carefully studied, a report will be sent to your consultant. Make sure you have been given an appointment to discuss the results.
PET scan for pancreatic cancer
A PET (Positron Emission tomography) scan will produce a three-dimensional, colour image of your body. It shows how well the tissues are working and can be used to help diagnose cancers.
Doctors can see the difference between scar tissue or an active cancer in the body.
A PET scan for pancreatic cancer can:
- Show whether there is a tumour present in the pancreas.
- Help to stage the cancer.
- Show whether the cancer has spread to other parts of the body.
- Help your specialists decide on the best treatment for you.
- Show how well the current treatment is working.
- Identify the difference between scar tissue and tissue that is cancerous.
What is a PET scan and how does it work?
PET scans are becoming more widely used in the NHS but they are still very expensive and only a few specialist hospitals in the UK have one.
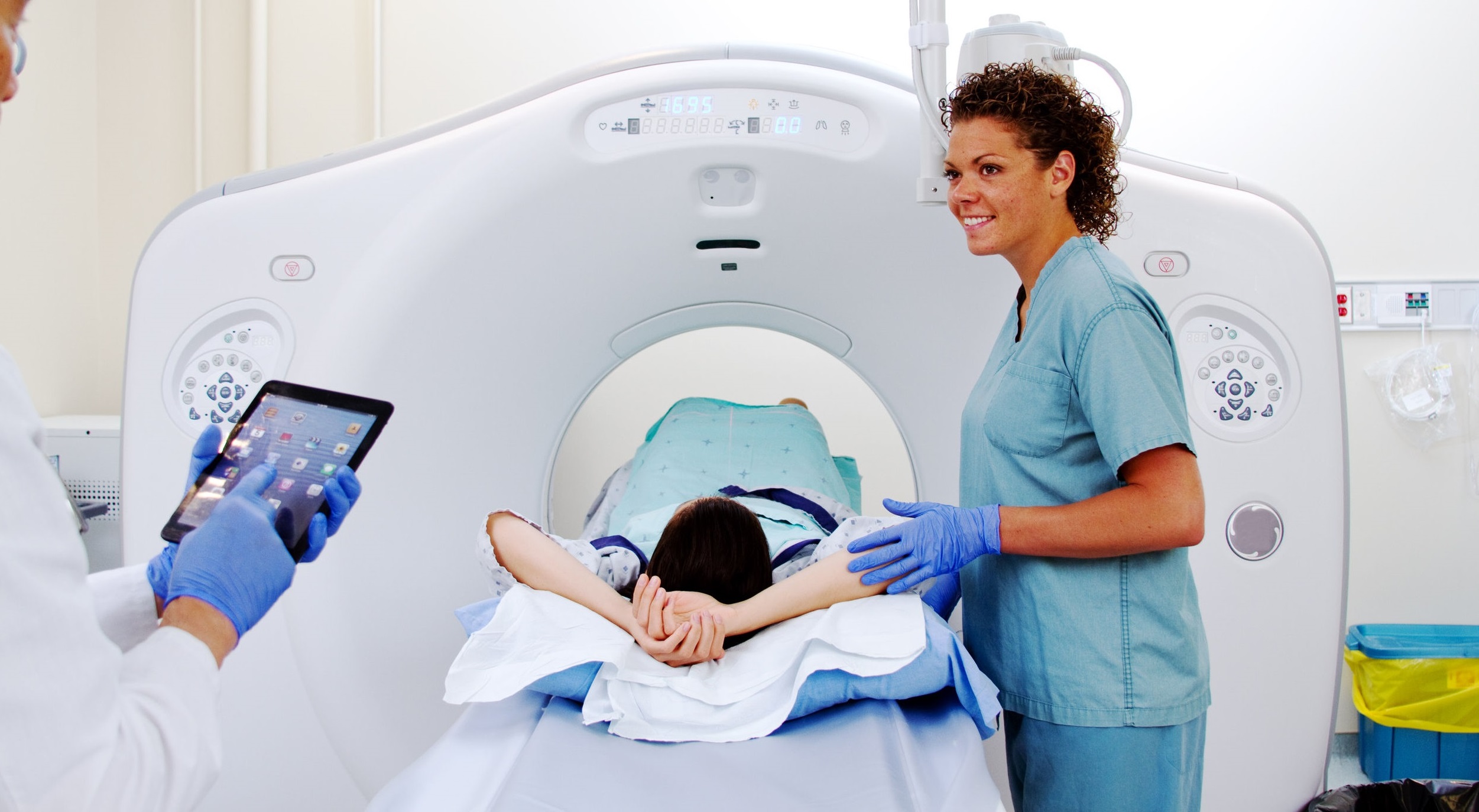
Patients may be asked to fast for about 4 to 6 hours prior to their screening. Radiographer will give you an injection of a very small amount of a harmless radioactive substance (radiotracer) alongside glucose, into a vein. You will need to wait for about 1hour while the radiotracer spreads through your body. You will then be asked to lie down on the flat bed of the scanner unit, which will move through the circular scanner at the end.
The radiotracer releases gamma waves (a form of radiation) that a camera in the PET scan can detect. When the dye and glucose are injected into the body, it travels to places where glucose is used for energy. Cancer tumours use glucose in a different way to normal tissue, and the PET scan shows these differences and can tell doctors whether cancer is present.
The radiographer will control the scan from outside the room and they will be able to see and talk to you. You will need to stay as still as possible while the scan is taking place.
The amount of radiation is very small (no more than you have during a normal X-ray) and it stays in your body for only a few hours.
Sometimes a CT scan can show that there may be cancer left after treatments such as chemotherapy. A PET scan can confirm whether it is active cancer or just scar tissue leftover as a result of treatments.
There are usually no side effects from this type of scan. It can take up to an hour to complete and you will need to lie still throughout the procedure.
Biopsy for pancreatic cancer
During a biopsy, a sample of tissue from the tumour is removed and looked at under a microscope to see if cancer cells are present. There are several types of biopsies that may be carried out for pancreatic cancer listed below. Your medical team will explain which procedure you need.
The most common methods of obtaining a biopsy for pancreatic cancer are:
Endoscopic retrograde cholangiopancreatography (ERCP).
flexible tube with a camera and other tools at its end (endoscope) is advanced fromthe mouth to the small intestine, near the pancreas. ERCP can collect images from thearea, as well as take a small biopsy with a brush.
Endoscopic ultrasound
Similar to ERCP, an endoscope is advanced near the pancreas. An ultrasound probe onthe endoscope locates the mass, and a needle on the endoscope removes some tissuefrom the mass.
Laparoscopy
This is a surgical procedure that uses several small incisions. Using laparoscopy, asurgeon can collect tissue for biopsy, as well as see inside the abdomen to determine ifpancreatic cancer has spread.
 The information provided in this site, or through links to other websites, is not a substitute for medical or professional care and should not be relied upon as such. Read our disclaimer.
The information provided in this site, or through links to other websites, is not a substitute for medical or professional care and should not be relied upon as such. Read our disclaimer.
Sources and references for this information product will be supplied on request. Please contact us quoting the Information Product number below:
| Information Product № | Published | 08/12/2022 | |
|---|---|---|---|
| Last Updated | 08/12/2022 | Next Review Due | 08/12/2025 |